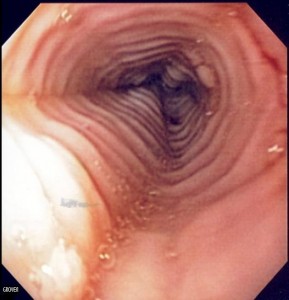
 Eosinophilic Oesophagitis (EoE), first described in the early 1990’s, has rapidly evolved as distinctive chronic inflammatory oesophageal disease. The diagnosis is based clinically by the presence of symptoms related to an oesophageal dysfunction and histologically by an eosinophil-predominant inflammation once other conditions leading to oesophageal eosinophilia are excluded. This striking male-prevalent[1] disease has an increasing incidence and prevalence in the westernised countries. Currently, EoE represents the main cause of dysphagia and bolus impaction in adult patients.[2]
Eosinophilic Oesophagitis (EoE), first described in the early 1990’s, has rapidly evolved as distinctive chronic inflammatory oesophageal disease. The diagnosis is based clinically by the presence of symptoms related to an oesophageal dysfunction and histologically by an eosinophil-predominant inflammation once other conditions leading to oesophageal eosinophilia are excluded. This striking male-prevalent[1] disease has an increasing incidence and prevalence in the westernised countries. Currently, EoE represents the main cause of dysphagia and bolus impaction in adult patients.[2]
Related to allergenic profile
EoE is an allergy-based disorder. It presents commonly in adults as long standing dysphagia, sometimes with food impaction.[3]
Topical corticosteroids lead to a rapid improvement of active EoE clinically and histologically; they are therefore regarded as first-line drug therapy. Elimination diets have similar efficacy as topical corticosteroids, but their long-term use is limited by compliance issues. Resolving the altered mucosal immune loss of tolerance offers a tantalising opportunity for natural resolution.
Findings
EoE, increasingly recognised in both adults and children, is characterised especially by oesophageal symptoms of dysphagia with impaction (a feeling of food being stuck at the lower end of the oesophagus) and biopsy evidence of significant eosinophil accumulation in the oesophageal epithelium.
Data collected so far suggest a multi-step allergy process starting with an atopic skin response that later primes the oesophagus on further allergen exposure – known as the ‘allergic march’, and which may be linked to thymic stromal lymphopoietin (TSLP).[4] Diagnosis of EoE is suggested by food impaction in a young adult with a personal and family history of allergy.
|
|||||||||||||||||||||||||||
| Table 2: Diagnostic criteria of Eosinophilic Oesophagitis. | |
| Clinical manifestations | Symptoms of oesophageal dysfunction |
| Histologic manifestations | Number of eosinophils >15 in at least one hpf |
| Exclusion criteria | Exclusion of GERD, clinically, endoscopically, histologically and if necessary by functional studies (e.g., pH-monitoring/impedance) Exclusion of other conditions that cause oesophageal eosinophilia |
| Adapted from Liacouras CA, et al. J Allergy Clin Immunol. 2011;128:3–20. | |
Nutritional Pearls
With respect to dietary counselling, the pearls that I would give you here are: when you talk to a patient with EoE, one thing that I use is the cardinal dysphasia diet. Explain the benefits of avoidance of anything that’s cut into anything other than a miniscule piece. The reduction of food mass especially food groups that are particularly notorious for catching in the oesophagus with a structural lesion such as EoE. Tough meat, doughy bread products, pasta — sometimes it will glom up and become very much of a bolus, rice, anything with a skin, like a potato skin, a fresh fruit or vegetable that’s raw and hard, those things are particularly likely to catch, so I just tell them, if you want a fresh fruit or vegetable, make sure it’s soft, cooked, and you cut it well. Those are dietary recommendations that I use routinely in all my EoE patients.
Next an exclusionary diet, or at least the exclusion of any recognised food allergens ahead of any clinical testing is worth undertaking as the benefits will be felt soon. Then, using digestive enzymes to aid in stomach and small intestinal degradation of antigens offers increased reduction in irritation.
TSLP inhibition through the inclusion of natural agent demonstrated in in-vitro studies to contribute to the suppression of the TSLP related allergic march are also worth exploring. These will include selenium, green tea, pineapple juice and berberine.[5],[6],[7],[8]
References
[1] Attwood SE, Smyrk TC, Demeester TR, Jones JB. Esophageal eosinophilia with dysphagia, a distinct clinicopathologic syndrome. Dig Dis Sci. 1993;38:109–16. View Abstract
[2] Hruz P, Straumann A, Bussmann C, Heer P, Simon HU, Zwahlen M, et al. Escalating incidence of eosinophilic esophagitis: A 20 year prospective, population-based study in Olten County Switzerland. J Allergy Clin Immunol. 2011;128:1349–50. View Abstract
[3] Dellon ES. Eosinophilic esophagitis: diagnostic tests and criteria. Curr Opin Gastroenterol. 2012 Mar 22. [Epub ahead of print] View Abstract
[4] Sherrill JD, Gao PS, Stucke EM, Blanchard C, Collins MH, Putnam PE, Franciosi JP, Kushner JP, Abonia JP, Assa’ad AH, Kovacic MB, Biagini Myers JM, Bochner BS, He H, Hershey GK, Martin LJ, Rothenberg ME. Variants of thymic stromal lymphopoietin and its receptor associate with eosinophilic esophagitis. J Allergy Clin Immunol. 2010 Jul;126(1):160-5.e3. View Abstract
[5] Moon PD, Kim HM. The suppression of thymic stromal lymphopoietin expression by selenium. Amino Acids. 2011 Nov 16. View Abstract
[6] Moon PD, Choi IH, Kim HM. Epigallocatechin-3-O-gallate inhibits the production of thymic stromal lymphopoietin by the blockade of caspase-1/NF-κB pathway in mast cells. Amino Acids. 2011 Aug 11. View Abstract
[7] Moon PD, Choi IH, Kim HM. Naringenin suppresses the production of thymic stromal lymphopoietin through the blockade of RIP2 and caspase-1 signal cascade in mast cells. Eur J Pharmacol. 2011 Dec 5;671(1-3):128-32. Epub 2011 Sep 24. View Abstract
[8] Moon PD, Choi IH, Kim HM. Berberine inhibits the production of thymic stromal lymphopoietin by the blockade of caspase-1/NF-κB pathway in mast cells. Int Immunopharmacol. 2011 Nov;11(11):1954-9. Epub 2011 Aug 19. View Abstract






5 Comments. Leave new
My 6 year old son was diagnosed with this condition a few years ago, it was discovered by accident while doctors were investigating his abdominal pain, he has had 3 major bowel operations and part of his bowel has been removed. He has recently started complaining of pain when swallowing food and says food is stuck in his throat, he also vomits quite often. Until now he has only been treated for reflux but is due to start treatment for eosinophilic oesophagitis next week, I have not been told what this treatment is or any side effects that he could have. I was wondering if anyone could tell me treatments for this condition, any information would be appreciated
Hi Lesley
Eosinophilic esophagitis (EoE) is a chronic inflammatory condition characterized by oesophageal dysfunction and eosinophilia infiltrate in the oesophageal epithelium in the absence of other potential causes of eosinophilia. EoE is increasing in incidence and prevalence, and is a major cause of gastrointestinal morbidity among children and adults. EoE is thought to be immune mediated, with food or environmental antigens stimulating a T-helper (Th)-2 inflammatory response. An increased understanding of the pathogenesis of EoE has led to the evolution of diagnostic and treatment paradigms.
3 major treatment options for EoE: pharmacologic therapy, dietary modification, and endoscopic dilation.
In 65% of children the exclusion of milk alone has resulted in resolution, but other triggering foods may also need to be removed and reintroduced to see if symptoms improve. As many children spontaneously recover from food allergy as their immune system matures, this may turn out to be a transitional therapy and represents a less traumatic intervention than dilation – steroids may offer some immediate relief but does not resolve.
The elemental diet had the highest success rate (> 95%), whereas the testing-based elimination diet (> 75%) and six-food elimination diet (> 70%) had lower success rates.
Spergel JM. Eosinophilic esophagitis in adults and children: evidence for a food allergy component in many patients. Curr Opin Allergy Clin Immunol. 2007 Jun;7(3):274-8. Review http://tinyurl.com/c77mtby
I hope that you find the recommendations include or are primarily directed at food exclusion and rotation.
My adult daughter had Eosonophilic Esophagitis diagnosed last year after several lengthy drastic attacks & numerous investigations.
She is just recovering from a second attack in two months. These attacks result in lengthy absence from work, serious weight loss & she has been admitted to hospital with dehydration.Her current medications & dietary restrictions are obviously not controlling this condition. Is there a specialist in the condition anywhere in UK who can help her return to a normal existence & contimue to work in a predictable manner.
Hi Maire
I was very disappointed to learn of the investigation, whilst this is less common in adults than children it is certainly a very well covered area in the literature.
You may have noticed that treatment can be a bit hit and miss, and I have no magic bullet. However, excluding the primary triggering foods, chewing well and eating small mouthfuls with regular slurps of water do offer some immediate relief. The use of steroids may also be required in an acute phase.
Foods most commonly involved are cow’s milk (74%), wheat (26%), egg (17%), soy (10%) and peanut (6%) but inhalant allergies may also be a strong factor. You need to find an allergist who is also skilled in gastroenterology. In the mean time this paper may offer you more ides.
• Ridolo E, Montagni M, Olivieri E, Rogkakou A, De’ Angelis GL, Canonica GW. Eosinophilic esophagitis: which role for food and inhalant allergens? Asia Pac Allergy. 2012 Oct;2(4):237-41. http://tinyurl.com/bje3ztd
Best wishes
Michael
I have finally been diagnosed with Eosinophilic esophagitis after over 7 years of suffering, with quite serious choking episodes. These resulted in me being hospitalised and taken to theatre numerous times, to have blocked foods removed. It was very scary, and in the beginning, the choking episodes happened twice a year, and became more frequent as the years went on, to the point where it was happening 3 times a week!!
I always knew something wasn’t right, but after years of tests in the ENT dept at my local hospital, I was told this was all in my head, and that I was telling myself I could not swallow, therefore causing me to choke!!!
I was so angry in the fact that they were assuming this, and the doctor actually wanted me to see a psychiatrist to get help! What absolute rubbish.
In the end I more or less diagnosed this condition myself after searching symptoms over the net, and after being finally referred to digestives dept ( instead of ENT ) at my local hospital for more tests, I finally got a diagnoses, to my relief and too prove I was not going mad!!
This condition, until diagnosed was upsetting my everyday life,with the constant choking and horrific heartburn. Certain foods seemed to trigger off the choking which were, beef, ( I no longer eat this) rice, potatoes and milk.
I believe it all started with bad symptoms of heartburn and acid reflux, which has left a lot of scarring.
I have since had the tight strictures in my esophagus broken whilst under anaesthetic, which will be a year ago this April, and so far it has worked a treat, and I have only had a few mild attacks. I am also using a steroid inhaler now, everyday.
Apparently I am the only patient to their knowledge being treated for this condition at my hospital, and although it seems quite rare, I think it is a condition, doctors do not know much about I the UK yet!
What I will say to anyone suffering these symptoms, is make sure you persue this and don’t give up until you finally get a diagnosis. Good luck!!